Concerning women’s health, female reproductive health is of utmost importance. Women’s bodies undergo hormonal and physiological changes from puberty to menopause, which are mostly determined by reproductive health. The reproductive system’s internal and exterior organs are included in this. Your mental, emotional, and social environments influence your reproductive health, just like they do other aspects of your health. It is beneficial to seek integrative medicine when seeking assistance and care for reproductive health concerns so that you may obtain holistic techniques that are most effective for you.
Female Reproductive Health: What Is It?
The whole well-being of the processes and functions that make up the female reproductive anatomy is defined by the WHO as female reproductive health. This covers social, mental, and physical components, with the notion that being healthy goes beyond simply not being ill or dysfunctional. Self-control and safety during sex and reproduction are essential components of female reproductive health.
Which issues related to female reproductive health are most prevalent?
Fallopian tubes, uterus, vagina, vulva, and ovaries are the reproductive organs of women. The pituitary gland, thyroid, adrenal glands, and hypothalamus are examples of secondary organs that are engaged in hormonal and functional activities.
You have the advantage of being sexually and reproductively viable when these systems function harmoniously and at their best. Some of the most frequent problems in female reproductive health are those that develop when imbalances, inflammation, or disease processes take place:
1. Impaired Sexual Functioning
Sexual dysfunction can be caused by pain, reduced reaction, or lack of desire during sex. This can happen at any time during a woman’s reproductive years, changing according on the circumstances and seasons of life. It’s vital to remember that sexuality is more than simply physical, and problems related to it might have hormonal, psychological, or societal roots. Low libido is the most common cause of female sexual dysfunction and can have a variety of medical and lifestyle consequences.
2. Unable to conceive
After a year of trying, 1 in 5 women in the US of reproductive age are unable to conceive. There are five primary reasons of infertility in women, according to the research. These consist of infertility that cannot be explained, infections, uterine and cervical problems, hormone imbalances, ovulatory abnormalities, structural problems, and infections. Premature ovarian insufficiency (POI), an ovulatory disorder, is a major cause for worry. It is a natural procedure for your ovaries to stop producing eggs at the age of 40. Some women may experience an early decline and early beginning of infertility as a result.
3. Fiberoroids
Eight out of ten women will have leiomyomas, commonly referred to as uterine fibroids, at some point throughout their lives. These appear as uterine growths, either internal or external, that are not malignant. While many women with this illness, the majority don’t have any symptoms. It is true that some women have severe and incapacitating symptoms, some of which might result in infertility.
4. The endometrial
The reproductive health of women is greatly concerned about this excruciating cyclical illness. When endometrial tissue—which is supposed to lining the uterus—is discovered outside of the uterus, endometriosis results. The ovaries, fallopian tubes, bladder, rectum, and abdominal cavity have all been documented to be invaded by this tissue. The endometrial tissue (both within and outside the uterus) sheds as hormones change in anticipation of implantation or menstruation. The whole non-intrauterine tissue loss will result in severe pain, inflammation, and crippling lifestyle effects.
5. Hypertension
Approximately 10% of females who are of reproductive age suffer from polycystic ovarian syndrome. This disorder of reproductive health has a disastrous effect on hormone control and metabolism. The rates of infertility, irregular menstruation, and endometrial hyperplasia are increased in women diagnosed with PCOS.
6. Cystitis interstitial
Women who are affected with bladder pain syndrome, sometimes referred to as interstitial cystitis (IC), experience persistent discomfort in the bladder and pelvic area. If you have infertility complex (IC), you are probably well-acquainted with the persistent desire to urinate and episodes of pelvic pain.
7. Diseases Spread Via Sexual Activity
Many women worldwide suffer from sexually transmitted infections. Many of these may be addressed and treated before they advance in the United States because to healthcare possibilities. Sometimes STDs can result in consequences like Pelvic Inflammatory Disease (PID). 3.7% of women between the ages of 14 and 49 have received PID treatment, according to the CDC. HIV and cervical cancer are two further problems associated to STDs that should be considered.
PCOD/PCOS
PCOD, also known as PCOS, is a disorder that affects women’s ovaries, which are reproductive organs that generate modest amounts of relaxin, inhibin, and male hormones known as androgens in addition to progesterone and oestrogen, which aid in controlling the monthly cycle.
Around 10% of women worldwide experience PCOD. Women with PCOS create more male hormones than usual compared to PCOD. They miss menstruation and have difficulty getting pregnant as a result of this hormone imbalance.
in addition to erratic hormone fluctuations, this illness can result in
1.Diabetes Inability to conceive
2.Acne Prolonged hair growth
It’s a somewhat prevalent illness for which there is no known cure.
PCOD:
The medical term for PCOD is Polycystic Ovarian Disease.
PCOD, or polycystic ovarian disease, is a medical condition in which a woman’s ovaries generate a large number of immature or partially mature eggs, which eventually develop into ovarian cysts. This results in enlargement of the ovaries and increased secretion of androgens, the male hormone responsible for infertility, irregular menstruation periods, hair loss, and abnormal weight gain. Changes in food and lifestyle can help manage PCOD.
PCOS:
The medical term for PCOS is Polycystic Ovary Syndrome.
PCOS (Polycystic Ovary Syndrome) is a metabolic disease that affects women who are between the ages of 12 and 51 and who have an imbalance in their hormones during their reproductive years. A rise in male hormones can cause women to miss their periods, experience irregular ovulation, which makes getting pregnant difficult, and experience abnormal facial and body hair development, all of which can eventually result in diabetes and heart disease. PCOS is a severe medical disorder that needs to be treated with appropriate care or surgery.
Many women are unaware that they have PCOD or PCOS. A set of symptoms that impact the ovaries and ovulation process include:
1.cysts on the ovaries
2. elevated masculine hormone levels
3. Missed or erratic intervals
What are the typical indications and symptoms of PCOD or PCOS?
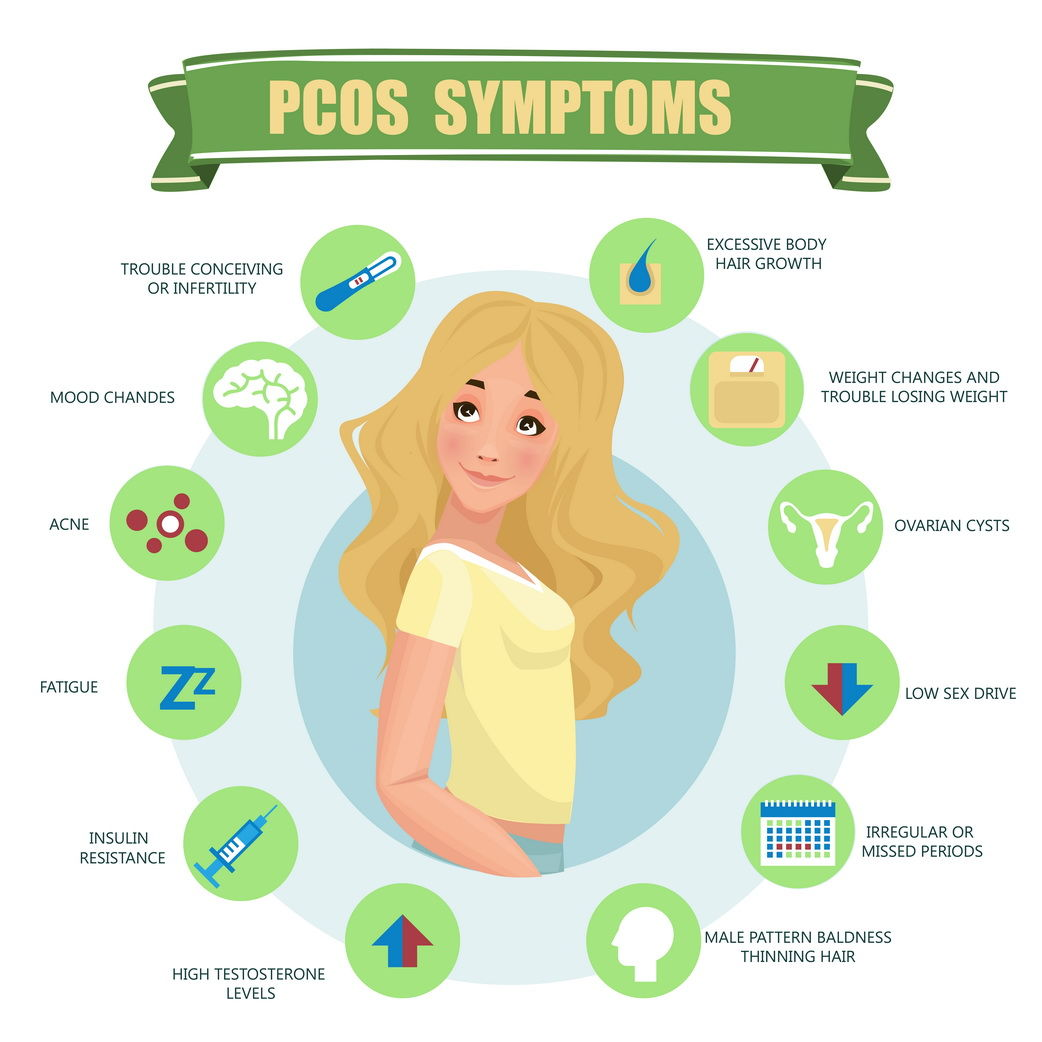
Some women initially notice symptoms around the time of their first menstruation, while others don’t notice symptoms until they’ve put on a lot of weight or are having difficulties getting pregnant. In females, the most typical indications and symptoms of PCOD Problem or PCOS are:
Menstruation irregularities (Oligomenorrhea)
Menstruation skipped or absent (amenorrhoea)
Menorrhagia, or heavy menstrual bleeding,
Overly Growth of hair on the face and body, including the back, belly, and chest
Acne on the upper back, chest, and face
Gaining weight
Hair loss (thinning and falling out of the scalp)
Darkening of the skin (behind the breasts, in the groyne, and on the neck)
PCOS causes
It is unknown exactly how PCOS affects women, although the following are some important contributing factors:
Overproduction of insulin: An excess of insulin in the body may lead to an increase in androgen production, a male hormone that is produced at a very low level in females and which interferes with ovulation.
Overproduction of androgen: The ovaries create excessive amounts of androgen hormones, which can cause hirsutism (the development of facial and body hair) and acne.
Low-grade inflammation: According to a recent study, women with PCOS have low-grade inflammation, which raises the production of testosterone and can result in cardiac problems or blood vessel problems.
Genetic Correlates: Women with PCOS have certain genetic markers
Problems related to PCOS/PCOD complications
Any woman who has PCOD or PCOS will wonder what happens to her body. Your health may be impacted by androgen levels that are greater than usual. The following are PCOS or PCOD issues that need to be treated by a doctor:
unusual bleeding in the uterus
Hypertension or infertility Unable to conceive
Diabetes type 2
Early delivery and preterm labour
Metabolic syndrome: an increased risk of stroke, heart disease, diabetes, high blood pressure, and blood sugar
Non-alcoholic steatohepatitis, or NASH
despair (Unwanted hair growth and other symptoms may lead to despair and anxiety in women)
Sleep apnea: This condition, which disrupts sleep at night by causing frequent breathing pauses, is more common in overweight women.
Endometrial cancer (caused by uterine lining thickening)
Miscarriage: the unplanned end of a pregnancy
The distinction between PCOS and PCOD:
It’s possible that some women are unsure about the similarities or differences between PCOD and PCOS. The symptoms of both medical diseases are similar and are linked to hormonal imbalances in women between the ages of 12 and 51 who are fertile. Here are several distinctions between PCOD and PCOS that all women need to be aware of:
PCOS/PCOD
1 PCOD is a prevalent condition that affects 10% of women worldwide.
PCOS is a severe medical disorder that affects 0.2% to 2.5% of women worldwide.
2 PCOD is a disorder in which the ovaries overproduce immature or partly developed eggs.
Hormonal imbalance, obesity, stress, and poor lifestyle choices are the main causes of this illness.
A more severe type of PCOS, known as anovulation, can cause the ovaries to cease producing eggs. PCOS is a metabolic condition.
3. Women with PCOD do not have reduced fertility; they can still ovulate and become pregnant on their own with minimal assistance, and they can carry their pregnancy to term with medication.
PCOS has a major impact on women’s fertility. Women with PCOS have irregular ovulation, which makes conception difficult. If they get pregnant, they run the danger of miscarrying, giving birth too soon, or having pregnancy problems.
4. There are no significant issues with PCOD.
Serious side effects of PCOS include type 2 diabetes, heart disease, hypertension, and, in later stages, endometrial cancer.
Modifying one’s lifestyle and using natural treatments for PCOS/PCOD
In females, PCOD/PCOS mostly impacts the hormone balance in the body. The actions listed below will assist women in lowering their body’s androgen levels:
1. Keeping a healthy weight: For women, a body mass index (BMI) of 18.5 to 24.9 is desirable and healthy; a BMI of 30 or more is obese and unhealthy. Sustaining a healthy body weight or decreasing weight can help lower blood pressure, lower the risk of heart disease, diabetes, and high blood pressure. It can also help maintain appropriate levels of androgen and insulin, which can help restore the menstrual cycle’s ovulation phase. See a nutritionist for advice on how to lose weight and get your BMI within a healthy range.
2. Reducing the amount of carbohydrates you eat: If you have PCOD or PCOS, stick to a diet high in complex carbohydrates or low in carbs to help keep your insulin levels stable. Consume seafood, meat, eggs, and naturally occurring fats such as butter, sesame seeds, pumpkin seeds, and sunflower seeds. Steer clear of sweets and starchy foods like potatoes, bread, rice, pasta, and beans.
3. Exercise frequently and stay active: Engaging in regular exercise and physical activity can assist in controlling blood sugar levels and maintaining a healthy weight if you suffer from PCOD or PCOS.
Identification of PCOD/PCOS
PCOD, also known as PCOS, is diagnosed by imaging and blood tests and involves physical symptoms that impact bodily systems. The gynaecologist will inquire about medical history, eating and drinking habits, and the use of any prescription or over-the-counter medications, including vitamins and supplements, depending on symptoms like irregular periods, unwanted male-pattern hair growth on a woman’s chest, face, and back, acne, or thinning of scalp hair.
In order to identify PCOS or PCOD, a gynaecologist could suggest:
1. Examining the reproductive organs physically to look for growths, anomalies, or lumps is called a pelvic examination.
2. Blood testing: A fasting lipid profile, which measures total cholesterol, high-density lipoprotein (HDL), triglyceride levels, and low-density lipoprotein (LDL), as well as glucose tolerance tests, are among the tests that may be used to better understand hormone levels.
3. Imagning test: Ultrasound imaging test to measure ovarian cysts, uterine lining, and ovarian size.
In addition to the aforementioned, the gynaecologist may suggest further testing to look for problems. These might consist of:
routine testing for triglycerides, cholesterol, glucose tolerance, and blood pressure
Anxiety and depression screening
obstructive sleep apnea (OSA) screening
What is the most effective course of therapy for PCOS or PCOD problems?
The goal of PCOD/PCOS treatment is to address your specific issues, such as hirsutism, acne, infertility, obesity, and irregular periods. Typically, lifestyle modifications such as nutrition, exercise, and weight loss come first in treatment. Even a small weight loss of 5 to 10 percent can help control your menstrual cycle.
The symptoms, such as hair growth, acne, and metabolic abnormalities, will determine the course of treatment.
This comprises:
Utilise medicine to control the menstrual cycle in order to address insulin resistance and hormonal imbalance.
Ovulation induction using oral medications and injections: controlling the number and quality of ovulation
Using fertility medications to treat infertility
reducing overgrowth of hair
Treatments for pigmentation and acne on the skin
When PCOS patients do not react to hormonal therapy, ovarian drilling is a laparoscopic surgery used to eliminate androgen-producing tissue in the ovaries.

MS. POOJA DEVI
ASSIST. PROFFESSOR, GIP
Related Posts
The Art of Negotiation: Effective Strategies for Achieving Win-Win Outcomes
Negotiation stands as a cornerstone skill in myriad contexts, ranging from business transactions and diplomatic relations to everyday interactions in personal and professional settings. At
: Azmostbet-aze45 Xətti Və Live At Azerbaijan Bukmeker:: Ruлиния Mostbet-aze45 И Live и Букмекерской Конторе Азербайджан Fairtrade Network Of Asia & Pacific Produc
: Azmostbet-aze45 Xətti Və Live At Azerbaijan Bukmeker:: Ruлиния Mostbet-aze45 И Live и Букмекерской Конторе Азербайджан Fairtrade Network Of Asia & Pacific Produce Казино Mostbet

Unveiling the Frontiers of Laser Physics
Introduction In the vast expanse of scientific exploration, few domains evoke as much intrigue and fascination as the realm of laser physics. With each passing

